Dry eye syndrome, also termed as dry eye disease, is a condition in which the eyes do not produce enough tears, or the tears that are produced are of unstable on cornea or the tear produced is poor quality. Some of the symptoms people experienced in dry eyes is feeling dry, discomfort, and itchy. Some of patients also experienced redness, irritation, and the foreign body sensations.
Dry eye syndrome is a common condition that affects any age people, but it is more commonly people over the age of 50 and women are more affected from dry eye syndrome. It can be caused by a various factors such as aging, certain medications used to treat acne, antidepressants, antihistamines, birth control pills, NSAIDs, Beta Blockers for controlling high blood pressure etc and certain medical conditions such as rheumatoid arthritis and Sjögren’s syndrome. It can also be caused by environmental factors, like dry air, staying long time in air conditional room or prolonged use of computers, gadgets and other screens.
If left untreated, dry eye syndrome can lead to more serious problems, such as corneal complications like keratitis or ulcers and scarring, which can affect your vision. So it is important to see an eye doctor if you are experiencing above mentioned symptoms of dry eye syndrome, so that the cause can be identified earlier and appropriate treatment can be started to minimise the further complications.
Table of Contents
Tests for Diagnosing Dry Eye Syndrome
Your eye doctors will always tests for diagnosing the dry eye syndrome while you visit them. Doctor may also ask you about your symptoms, medical history, and perform a physical examination of your eyes to help diagnose dry eye syndrome using the commonly used following tests.
Schirmer test
The Schirmer test is a simple and quick test that is used to measure the amount of tears that are produced by the tear glands (lacrimal glands). This tests can be performed by two types
- Schirmer’s test without anesthesia
- Schirmer’s test with anesthesia (Using eye drop for anesthesia)
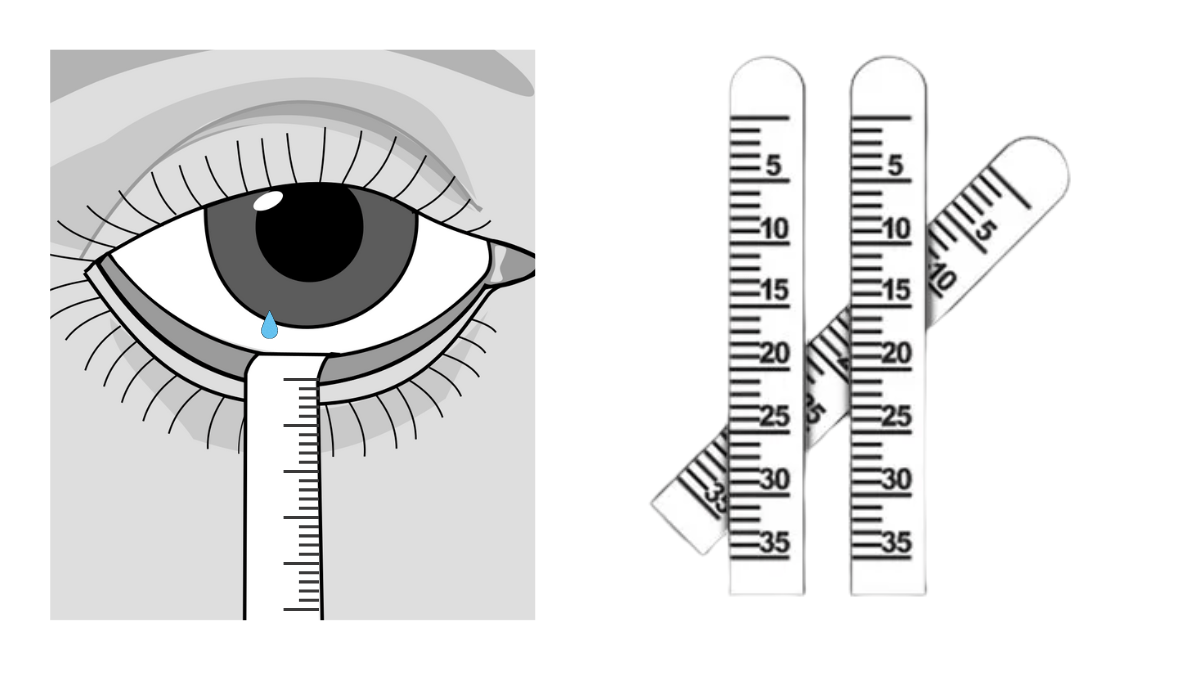
Most common test is Schirmer’s test without anesthesia which help to assess the aqueous tear production by placing the Schirmer’s strip, made up of Whatman no. 41 filter paper with dimension of 5 mm x 35 mm. The initial 5 mm of the Schirmer strip will folded and placed placed under the lower eyelid (at the junction of the lateral one third and medial two third of the lower fornix ) and it will keep there for 5 minutes. The amount of tears that are absorbed by the strip at the end of 5 minutes is then measured.
Less than 15mm in Schirmer test result may indicate that the eyes are not producing enough tears, which can be a sign of dry eye syndrome. Your eye doctor will also ask you for other tests if needed to confirm the diagnosis of Dry eyes.
Schirmer’s test with anesthesia will done usually 15 minutes after the initial test in which basal secretion will measured. Topical anesthesia eye drop will installed into the eyes and after 2 minute of anesthtic eye drop installation excess anesthetic drop will be wiped off and then schirmer strip will be placed in same manner as mentioned above and keep it for 5 minutes and the measurement will be record.
Schirmer tear test value grading
In general, the following grades are often used to interpret the results of the Schirmer tear test for diagnosing dry eye syndrome. (Mishra et al., 2022)
- More than 15 mm: Normal
- 10-15 mm: mild dry eye
- 5-10 mm: moderate dry eye
- Less than 5 mm: severe dry eye
Tear break up time (TBUT)
The tear film breakup time (TBUT) also known as tear film break-up time (TFBUT) test is another commonly performed test for dry eye to diagnose. It is very simple and quick test which is used to measure the stability of the tear film on the surface of the eye. The tear film is a thin layer of tears that coats the surface of the eye and helps to keep it moist, comfortable and help to maintain optical transparency for clear vision.
To measure TBUT, drop of fluorescein is instilled into the patient’s eyes and the patient is asked not to blink while the tear film is observed by Slit lamp under a broad beam of cobalt blue illumination. The eye doctor then asks the person being tested to blink a few times first and then looks at the eye through a slit lamp. The TBUT is recorded as the number of seconds that elapse between the last blink and the appearance of the first dry spot in the tear film. A Tear break up time under 10 seconds is considered abnormal.
If patient also have other sign in cornea such as punctate epithelial erosion (PEE) and visible after the stain with fluorescein, it is also considered as another sign of ocular surface dryness.
A shorter tear film break up time may indicate that the tear film is not stable and is breaking up too quickly, which can be a sign of dry eye syndrome. However, it is important to note that the normal range may vary depending on factors such as age, gender, and overall health conditions.
Conjunctival staining test
The conjunctival staining test also another test for diagnosing dry eye syndrome. It is a diagnostic procedure that involves applying a dye to the conjunctiva and examining the conjunctiva structure for any changes. This test is used to identify irritation or inflammation of the conjunctiva and can help to diagnose a variety of eye conditions, including dry eye syndrome, allergic conjunctivitis, and other types of eye infections. According to a study in the American Journal of Ophthalmology, Schirmer 1 testing and conjunctival staining with lissamine green are critical tests to include when screening dry eye patients for possible Sjögren’s syndrome.
Other Tests for Diagnosing Dry Eye Syndrome
- Tear Osmolarity Test
- Matrix Metalloproteinase-9 Test
- Meibography
- Interferometry
- LipiScan™ Dynamic Meibomian Imager (DMI)
- Matrix Metalloproteinase 9 Testing
References:
- Mishra, S., Bista, B., Basnet, P., Chaudhary, P., Chaudhary, S., Gupta, S., & Bista, P. R. (2022). Evaluation of tear secretion and tear film stability in patients with pterygium and normal individuals. Med Phoenix, 7(1), 14–18. https://doi.org/10.3126/medphoenix.v7i1.47347



