Grading in ophthalmology is an important tool to grade the eye diseases severity. The grading system develops over time, These grading systems in ophthalmology are useful for resident doctors, postgraduate students, optometrist, ophthalmic assistants which will help them in preparations of various examinations and the initial phase of their clinical practice for systematic management of various ophthalmology cases.
Some grading systems which is used commonly in Ophthalmology are as follows.
Table of Contents
Grading of Ptosis
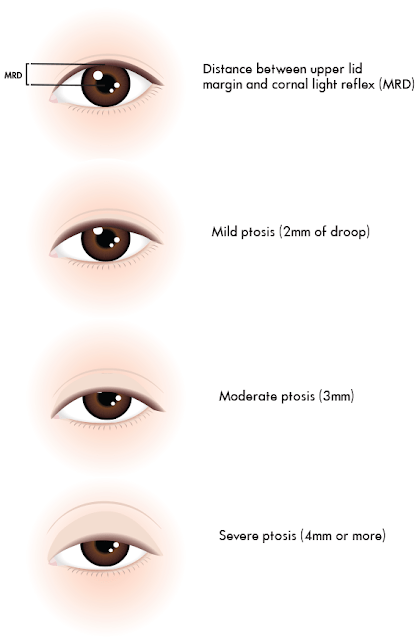
Ptosis is a drooping of the upper eyelid. While grading ptosis of an eyelid we have to measure Marginal Reflex Distance MRD (Distance between Upper lid margin and corneal light reflex), as based on the MRD ptosis can be grade as follows.
- Mild Ptosis: 2mm of drop
- Moderate Ptosis: 3mm of drop
- Severe Ptosis: 4 mm or more dropping of the upper eyelid.
Grading of Entropion
Entropion is a condition where the lid margin is inturned. Depending on the degree of inturning, dividing into three grades according to Kemp and Collin Classification.
Grade 1: only the posterior lid border is inrolled.
Grade 2: inturning of the intermarginal strip.
Grade 3: whole lid margin including anterior border inturned
Grading of Ectropion
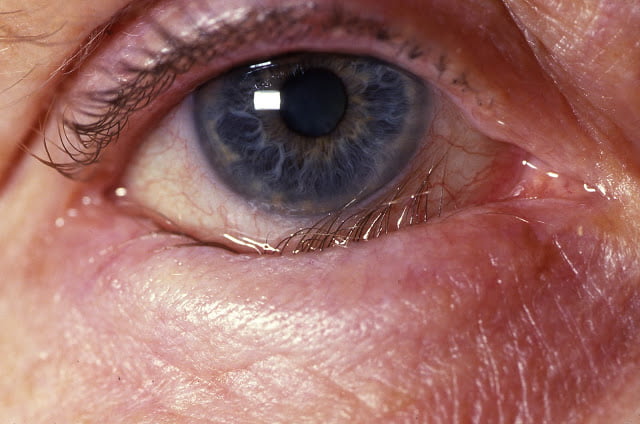
Ectropion is an outward rolling of the lid margin.
Grade 1: The only punctum everted
Grade 2: Lid margin is everted and palpebral conjunctiva is visible.
Grade 3: Fornix is visible
Hyphema | Ophthalmology Grading
Hyphema is the medical term that defines the blood in the anterior chamber of the eye. Hyphemas can be graded from grade I-IV. (Source AAO)
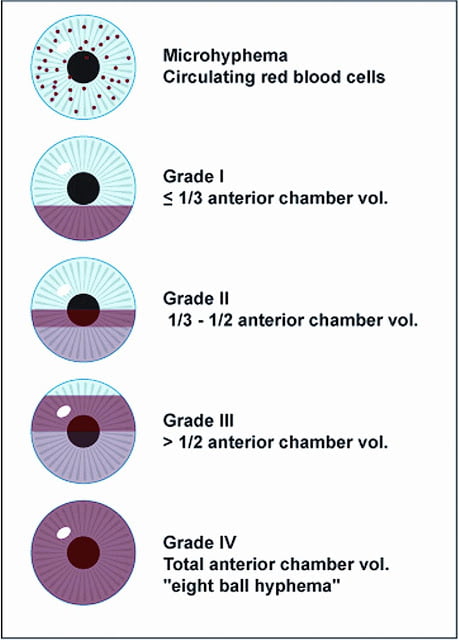
Grade 0: No visible layering, but red blood cells (RBCs) within the anterior chamber (microhyphema)
Grade I: Layered blood occupying less than 1/3 of the anterior chamber
Grade II: Blood filling 1/3 to 1/2 of the anterior chamber
Grade III: Layered blood filling ½ to less than total of the anterior chamber
Grade IV: Total clotted blood, often referred to as blackball or 8-ball hyphema
Anterior Chamber: AC Cells Grading
As based on Standardization of Uveitis Nomenclature (SUN).
| Grade | Cells in field (1*1mm Slit Beam) |
| 0 | <1 |
| 0.5+ | 1-5 |
| 1+ | 6-15 |
| 2+ | 16-25 |
| 3+ | 26-50 |
| 4+ | >50 cells |

AC Flares
Anterior chamber flares were graded as follows, based on the SUN grading system.
- 0 Complete absence
- 1+ Faint flare (barely detectable)
- 2+ Moderate flare (iris and lens still clear)
- 3+ Marked flare (iris and lens hazy)
- 4+ Intense flare (coagulate aqueous, no circulation, fibrin visible).
Van Herick’s AC Depth Grading
The Van Herick technique is an eye examination method used to determine the size of the anterior chamber angle of the eye. The peripheral anterior chamber depth (PACD) is compared to the adjacent corneal thickness (CT) and the presumed angle width is graded as follows:
- Grade 4 (Wide open angle): PACD = 3 / 4 to 1 CT
- Grade 3 (Mild narrow angle): PACD = ¼ to ½ CT
- Grade 2 (Moderate narrow angle): PACD = ¼ CT
- Grade 1 ( Extremely narrow angle): PACD < ¼ CT
- Grade 0 (closed angle): PACD = Nil
Cataract Grading
Many ophthalmology residents face difficulties while grading cataract. Here we are discussing, How to grade cataracts?
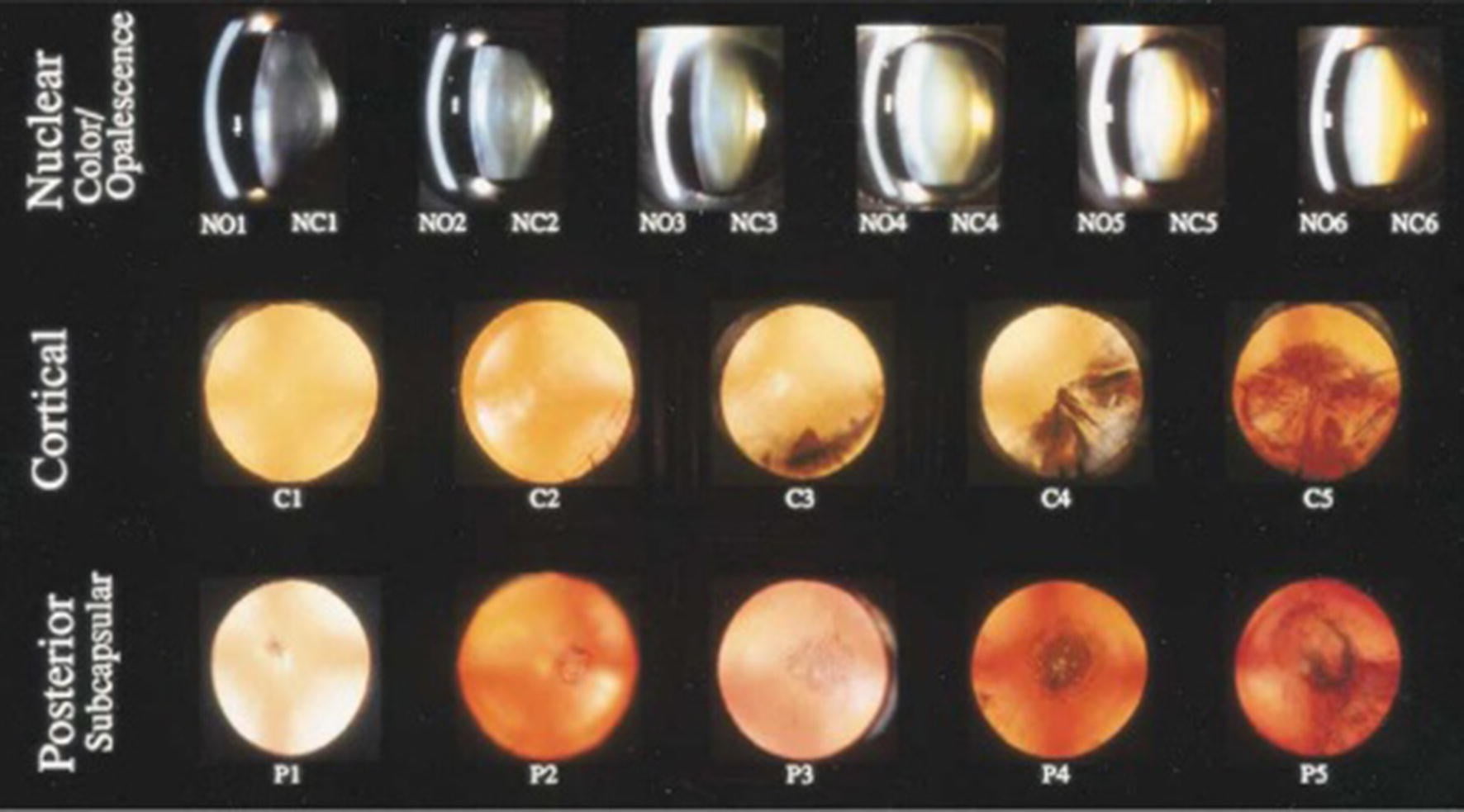
Nuclear Sclerosis Grading
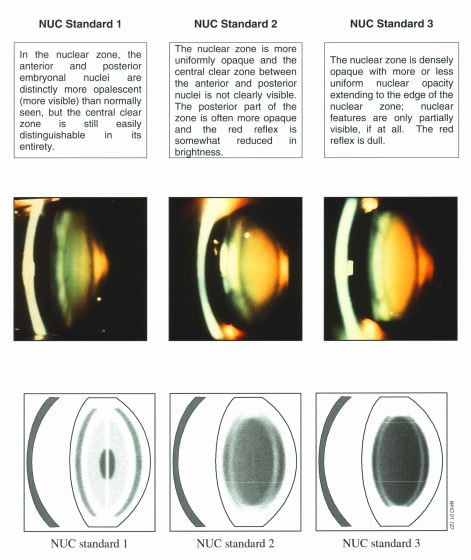
Nuclear sclerosis (NS) grading of nuclear cataract. It is the cloudiness of the nucleus, the central portion of the crystalline lens. It can be graded as per the color of the nucleus after dilation of the pupil.
NS tr or 1+: Nucleus clearer than anterior/posterior sections.
NS 2+: Nucleus equal to the anterior/posterior sections (same opacity level throughout).
NS 3+: Nucleus denser than anterior/posterior sections.
NS 4+: Brunescent: Cataract completely opaque/brown.
Cortical Cataract Grading
For Cortical cataract grading use retroillumination techniques on the slit lamp. A relatively short and broadly focused beam, positioned within the 3 or 9 o’clock border of the pupil, should be used. If it is not possible to illuminate the pupil uniformly to give a red reflex, the beam should be moved so that eventually all areas can be examined against the red reflex.
In normal cases, the lens is transparent in retroillumniation.
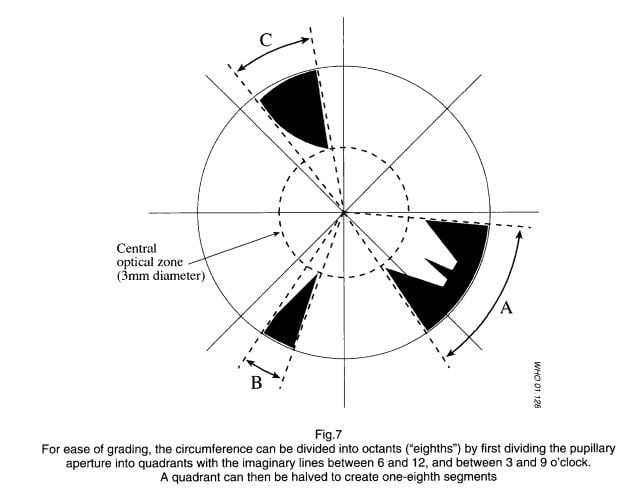
- Cortical Opacity 1: If cataract involves one-eighth ⅛ but lens than a quarter ¼ of the circumference.
- Cortical Opacity 2: If cataract involves a quarter 1/4 and less than half 1/2 of circumference.
- Cortical Opacity 3: Involves Half of the circumference or more than half.
The Lens Opacities Classification System : Ophthalmology Grading
Posterior Sub Capsular Cataract Grading
PSCC grading also done by slit-lamp using retroillumination. Posterior Sub Capsular Cataract (PSCC) is located just in front of the posterior capsule of the crystalline lens. PSC is grading according to vertical diameter in mm. The observer will measure the vertical height of the PSC cataract and grade it as follows based on the WHO Cataract grading system.
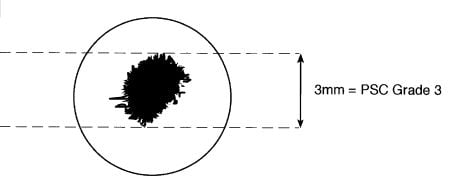
PSC 0: Less than 1 mm
PSC 1: 1 mm to less than 2 mm
PSC 2: 2 mm to less than 3 mm
PSC 3: more than 3 mm
Posterior Capsular Opacification Grading
Posterior capsule opacification (PCO), also known as “after cataract” is mostly seen after cataract surgery. The posterior capsule of the lens undergoes secondary opacification due to the migration, proliferation, and differentiation of lens epithelial cells. Nd: YAG laser is the most modern tool to treat
PCO and has a high success rate.
The EPCO grading scale
- Grade 0 (None): Transparent of Capsule
- Grade 1 (Minimum): Wrinkling of the capsule with a fine layer of LECs
- Grade 2 (Mild): Honeycomb PCO; a thicker layer of LECs with dense fibrosis
- Grade 3 (Moderate) Classical Elschnigg pearls and of a very thick layer of LECs
- Grade 4 (Severe): Very thick Elschnigg pearls, severe opacity with a darkening effect
LECs = lens epithelial cells; PCO = posterior capsule opacification
PCO scoring by slit-lamp derived reflected light photographs and retroillumination.

- Grade 0: PCO do not intrude on the intraocular lens (IOL) edge.
- Grade 1: PCO intrudes less than half of the IOL edge area and below the continuous curvilinear capsulorhexis (CCC) margin.
- Grade 2: PCO intrude more than half of the IOL edge area and below the CCC margin.
- Grade 3: PCO intrude the CCC margin but do not intrude visual axis
- Grade 4: PCO intrude visual axis’. ‘Visual axis’ means ‘3 mm from the centre of the pupil.
Diabetic Retinopathy Grading
Diabetic Retinopathy grading is done as per the finding on ophthalmoscopy examinations such as Microaneurysms, dot haemorrhage, blot haemorrhages, cotton wool spots, intraretinal microvascular abnormalities (IRMA), neovascularization and vitreous/pre-retinal haemorrhages.

Hypertensive Retinopathy Grading
Keith-Wagener-Barker Classification of Hypertensive Retinopathy
Grade I: Mild generalized retinal arteriolar narrowing
Grade 2: Definite focal narrowing and arteriovenous nipping
Grade 3: Signs of grade 2 retinopathy plus retinal haemorrhages, exudates and cotton wool spots
Grade 4: Severe grade 3 retinopathy plus papilledema
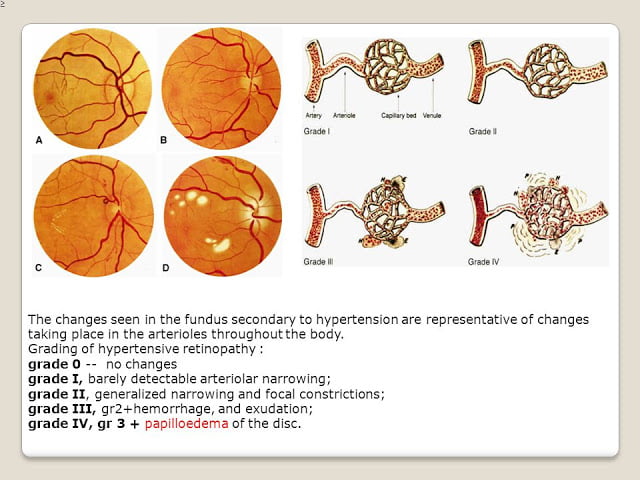
Wong and Mitchell Classification of Hypertensive Retinopathy
Mild: 1 or more of the following signs: generalized arteriolar narrowing, focal arteriolar narrowing, arteriovenous nicking, arteriolar wall opacity
Moderate: 1 or more of the following signs: retinal haemorrhage (blot-, dot-, or flame-shaped), microaneurysm, cotton wool spots, hard exudates
Severe: Moderate retinopathy plus optic disc swelling
Relative Afferent Pupillary Defect (RAPD) Grading
The ‘swinging light test’ is used to detect a relative afferent pupil defect (RAPD).
1+: Weak initial constriction followed by greater redilation
2+ Initial pupillary stall followed by greater redilation
3+ Immediate pupillary dilation
4+ No reaction to light
Papilledema Grading
Modified Frisen Scale for Papilledema
Grade 0: Normal optic disc
Grade I: Minimal papilledema: subtle C-shaped halo of disc edema with a normal temporal disc margin
Grade II: Low-degree papilledema: circumferential halo of disc edema
Grade III: Moderate papilledema: obscuration of one or more segments of the major blood vessels leaving the disc.
Grade IV: Marked papilledema: partial obscuration of a segment of major blood vessel on the disc.
Grade V: Severe papilledema: partial or total obscuration of all blood vessels on the disc
Vitreous Haze Grading
NIH grading system for vitreous haze in uveitis
- Grade 0.5, trace haze
- Grade 1: clear disc and vessels, hazy Retinal Nerve Fibre Layer
- Grade 2: hazy disc and vessels
- Grade 3: optic disc visible
- Grade 4: optic disc not visible
Vitreous Cells Grading
Based on NIH Grading System
| Grade | Vitreous cell |
| 0.5+ | 1-10 |
| 1+ | 11-20 |
| 2+ | 20-30 |
| 3+ | 30-100 |
| 4+ | >100 |



