Table of Contents
Introduction
Slit Lamp = Slit beam of light
Biomicroscope = Biological living tissue i.e. the eye
Slit Lamp Biomicroscope consists of a Compound Binocular Microscope & an Illumination System – typically linked on a common pivot so that the illumination & viewing systems are focused on the same plane. It provides the examiner with a stereoscopic (i.e. three dimensional) view of the eye. The slit-lamp instrument was developed by Prof. Allvar Gullstrand (1862-1930)
Types of Slit Lamp
There are two types of Slit Lamp Biomicroscope available on market on the basis of a model. They are as follows
- Zeiss Type
- Haag Streit Type

Zeiss Type: In this model slit lamp the light source is at the base of the instrument
Haag Streit Type: In the Haag Streit model the light source is at the top of the instrument.
On the basis of the Illumination System, it can be categorized as LED or Halogen slit lamps.
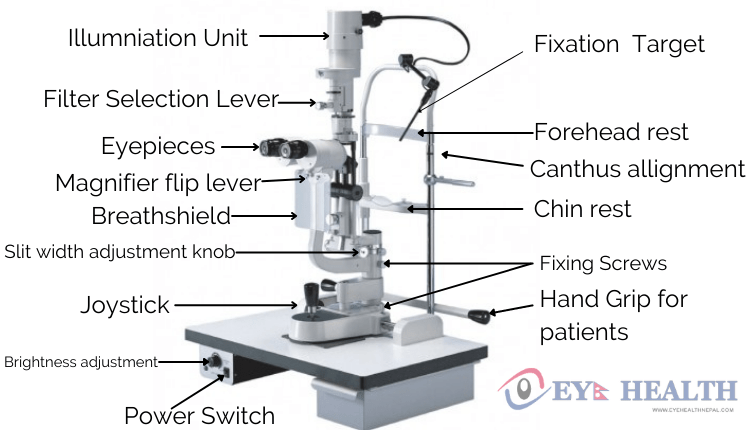
Slit Lamp Parts
It consists of 3 main parts.
- Mechanical Support System
- Illumination System
- Observation System
1. Mechanical Support System
The mechanical support system consists of the following parts.
- Fixation target
- Forehead band
- Chinrest
- Handgrip
- Fixing Screws for locking slit lamp
- Adjustment knobs
- Joystick
- Power switch
2. Illumination System
- Lamp Housing Unit (Light source Halogen/LED bulb)
- Condensing Lens
- Slit Apertures
- Filters
- Projection Lens
- Reflecting Mirror or Prisms

3. Observation System
The observation system consists of the followings
- Compound Microscope & Binocular Eyepieces
- Magnification Changer
- Porro-Abbe Prism

Other Types of Slit Lamp
Apart from Regular Slit Lamp, there are different types of handheld Slit Lamp devices, which are used for disabled, Infants or in bedbound patients.
Associated Accessories
- Applanation Tonometer
- Co observation tube
- Gonioscopic lens
- Digital archiving devices
- 90D/78D lenses
- Lasers
Examination Procedure
Instrument Setting: Illumination System & Observation System should be coupled & adjusted according to Individual Observer
Eyepiece Adjustment: Use Focusing Rod (Provided with Slit Lamp) for eyepiece adjustment
Bring Slit Beam in Sharp Focus by Rotating the Eyepiece Anticlockwise (+Side) & then Clockwise to get the sharp focus for the first time. Make sure you are able to view through the eyepieces binocularly.
Patients Position
- Explain patient what you are going to do with the Slit Lamp.
- Make sure he/she is seated comfortably.
- Ask him/her to keep his chin on the chinrest & rest his forehead against the forehead band.
- Align the outer canthus of the patient to the central marking by adjusting the chinrest up and down.
On Patient Focusing Check
- Focus the light on the patient’s closed lid.
- Rotate the illumination side to side.
- If the light remains stationary, then the instrument is correctly focused.
- If light shows any relative movement then the instrument is out of focus.
Tips: Start with Low Magnification & Diffuse Illumination while examination.
Slit Adjustment: The width & the height of the slit lamp can be adjusted.
- Orientation of the slit is possible in all angles.
- In some Slit Lamp, there is a graticule to measure any lesions.
- Without the graticule, the slit width & height along with its angle is measurable from the scale.
SLIT-LAMP BIOMICROSCOPIC EXAMINATION PROCEDURE
While examining the patient in slit lamp you must have to follow the chronological orders that mean you have to start examining from the outermost part eyelids and eyelid margin at first and slowly go to posterior parts of the eyeball.
Eyelids and Eyelid margin examination
- Examine the Superior Temporal Eyelid & Lashes – Using Scanning (to-and-fro) motion i.e forward and backward movement.
- Can be easier with the patient’s eye closed
- Examine Inferior Lid & Lashes in the same manner while also examining Lid apposition to the eye & meibomian gland appearance
- Assess the lid for anomalies including abnormal lid position ( Eg; Ptosis, Entropion, Ectropion), Redness, Inflammations, Ulcers & Growths.
- Inspect the lashes for colour (Eg. White), areas where lashes are missing or misdirected & presence of scales
Tear film Assessment
For the Assessment of the Tear Meniscus, the height of the slit beam is decreased to 1 mm. Then judging the relative height of the Meniscus at the lower lid margin as a proportion of the beam height.
Conjunctiva and Sclera examination
- Ask the patients to look upwards – while pulling the lower eyelid gently downward to expose the lower fornix for examination.
- Examine both the bulbar and palpebral conjunctiva using the scanning process.
- Next ask the patient to look downwards and gently pull up the upper eyelid, thereby exposing the superior bulbar conjunctiva for examination.
- Finally, ask the patient to look in right and the left gaze to allow examination of the entire conjunctiva, caruncle along the sclera.
Anterior Chamber
Examine Iris by moving the joystick towards the patients. The Iris should come into focus. Use scanning process under direct Illumination methods. Also, observe the depth of the anterior chamber. Note any findings seen.
Lens and Cataract Examination
The pupil must be dilated before examination of the lens and cataract. Use direct illumination with Parellelpipped or Optic Section
For Non-Dilated Pupil
Illumination angle – reduced until an optical section of the lens is seen. This may be 15 degrees for elderly patients with a small pupil.
Direct Illumination is useful for cortical cataracts as it can show large amounts of lights scatter due to background light scatter & reflection that does not cause vision loss
Retro Illumination from the fundus is more useful in evaluating posterior subcapsular cataract & cortical opacities.
Vitreous
Moving the joystick further towards the patient allows viewing of the vitreous with a parallelepiped when the pupil is dilated. To look for anterior vitreous floaters, it can be useful to ask the patients to look up, down and straight Ahead, So that the opacities become visible as they float through the field of view.
Retina / Optic Nerve Head Examination
Use additional accessories like 90 D or 78 D lenses by placing them at the front of the eye to be examined. Slowly move the joystick away from the pt. for the correct focus
Slit Lamp illumination techniques
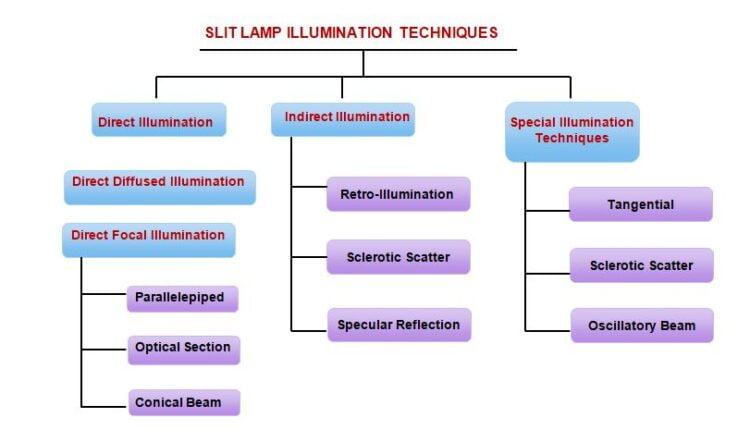
Direct Diffused Illumination
Broad beam opened, unfocused light beam, directed obliquely between 30 – 45 degree, Low magnification such as 10X. It is used for a general gross overview of eyelid, lashes and anterior segment of the eye,
Sclerotic scatter
Done with 10x magnification. In this techniques, a tall, wide beam is directed straight at the limbus at an angle of 45 – 60 degree. The light is scattered through the cornea to reveal a general pattern of opacities. Total Internal Reflection of the incoming light at inner corneal boundaries (Endothelium & Epithelium).
Applications: scars, foreign bodies, corneal defects, irregularities in the Cornea.
Retro-Illumination
This technique is used to observe Media Clarities & Opacities. The slit beam and microscope are made co-axial and light strikes the fundus and creates a glow behind the opacity in the media. The media opacity creates a shadow in the glow.
Uses Abnormalities in the anterior vitreous, lens, anterior Chamber, corneal opacities and media opacities.

Slit Lamp filters
- Cobalt Blue Filter: Blue filled circle filter is used to enhance the view of fluorescein dye in the tear film of the eye. Typically used for Fluorescein Staining & Goldmann Applanation Tonometry

- Red Free filter: Symbol is Green Filled Circle: Used to enhance the view of blood vessels and haemorrhages
- Neutral Density filter: Symbol is Circle with Hashed Lines: Used to decrease maximum brightness for photosensitive patients.
- Yellow Filter: Yellow filled Circle symbol in slit lamp located in the Observation system: Used for good contrast enhancement when using fluorescein & the Cobalt Blue Filter
- Grey: Circle with Thick Line: It Decreases Maximum Brightness for Photosensitive Patients
- Heat Absorbing filters are built into most slit lamps it helps to decreases patient discomfort during slit lamp examinations.